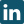New research shows that a new and unique approach to cancer immunotherapy may improve survival in patients with mesothelioma and ovarian cancer. Immunotherapy is used to stimulate the body’s immune system against cancer. For example, according to the Merck Manual Home Health Handbook, vaccines comprised of antigens derived from tumor cells can boost the body’s production of antibodies or immune cells (T lymphocytes). Extracts of weakened tuberculosis bacteria (which are known to boost the immune system) have been successful when introduced into the bladder to prevent bladder tumors.
Now, a team of researchers with the Massachusetts General Hospital (MGH) Vaccine and Immunotherapy Center report that “a protein engineered to combine a molecule targeting a tumor-cell-surface antigen with another protein that stimulates several immune functions, slowed tumor growth and prolonged survival in animal models of both tumors.” The team, which includes senior author of the report and Director of the MGH Vaccine and Immunotherapy Center Dr. Mark Poznansky, created a vaccine that stimulates a patient’s own dendritic cells, rather than utilizing the standard approach that requires “extracting a patient’s own immune cells, priming them with tumor antigens and returning them to the patient,” says Poznansky. Dr. Poznansky adds that the latter process is considered complicated and costly, and offers a poor prognosis.
The body’s dendritic cells are antigen presenting cells that, according to the National Center for Biotechnology Information (NCBI), mediate several physiologic components of immunogenicity (the ability to produce an immune response) such as the acquisition of antigens in tissues, the migration to lymphoid organs, and the identification and activation of antigen-specific T cells.
According to the study, the MGH team’s approach begins with the engineered protein, which in this case fuses an antibody fragment targeting a protein called mesothelin — expressed on the surface of such tumors as mesothelioma, ovarian cancer and pancreatic cancer — to a protein from the tuberculosis bacteria that stimulates the activity of dendritic and other immune cells. In this system, the dendritic cells are activated and targeted against tumor cells while remaining inside the patient’s body.
The team concluded that the mesothelin-targeted fusion protein attaches to mesothelin on mesothelioma (or ovarian cancer) cells, then activates dendritic cells, and enhances the cells’ processing and presentation of several different tumor antigens, inducing a number of T-cell-based immune responses.
In animal studies including both types of tumors, treatment with the fusion protein slowed tumor growth and extended survival significantly. The team concluded that this is likely the result of the activity of cytotoxic CD8 T cells. Cytotoxic CD8 T cells monitor all the cells of the human body. They are equipped to destroy any others that express foreign antigen fragments in their class I molecules.
The MGH team notes that, like other types of immunotherapy, this innovative cancer vaccine is nontoxic, it may offer a better survival rate than other vaccines, it’s a lower cost approach to treating cancer, and it even has the potential to lower the risk of cancer recurrence. Researchers also believe that in the future this approach could ultimately be used to target any type of cancer.
Sources
- American Cancer Society
- Kimball’s Biology Pages
- Massachusetts General Hospital (MGH)
- National Center for Biotechnology Information (NCBI), U.S. National Library of Medicine (NLM)
- Science Daily
- Photo by Nephron (Own work) [CC-BY-SA-3.0 or GFDL], via Wikimedia Commons
- Journal Reference
- Jianping Yuan, Satoshi Kashiwagi, Patrick Reeves, Jean Nezivar, Yuan Yang, Nadiah Arrifin, Mai Nguyen, Gilberte Jean-Mary, Xiaoyun Tong, Paramjit Uppal, Svetlana Korochkina, Ben Forbes, Tao Chen, Elda Righi, Roderick Bronson, Huabiao Chen, Sandra Orsulic, Timothy Brauns, Pierre Leblanc, Nathalie Scholler, Glenn Dranoff, Jeffrey Gelfand, Mark C Poznansky. A novel mycobacterial Hsp70-containing fusion protein targeting mesothelin augments antitumor immunity and prolongs survival in murine models of ovarian cancer and mesothelioma. Journal of Hematology & Oncology, 2014; 7 (1): 15 DOI: 10.1186/1756-8722-7-15